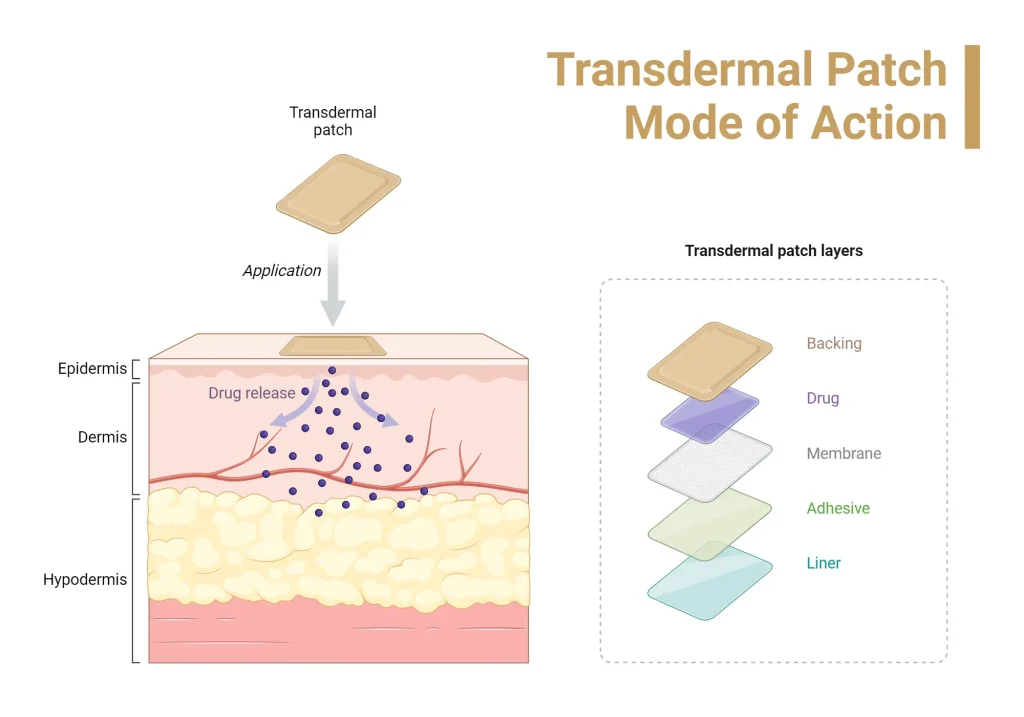
Transdermal patches offer a discreet, effective way to deliver medicine through the skin, a cornerstone of modern patch-based therapies. By delivering drugs across the skin rather than through the digestive system, they can provide steady levels over hours or days. This article introduces what transdermal patches are, how transdermal patches work, and how they fit into patient care. There are types of transdermal patches, including nicotine, fentanyl, and hormone options, each designed for a different therapeutic goal. We also review care and safety of transdermal patches to minimize risks.
Beyond the familiar terminology, readers encounter skin-applied drug delivery and percutaneous systems that move medicine through the surface layers. Other terms include dermal patch, topical delivery device, or transdermal patch substitute, all aimed at steady blood levels with comfort. Considering benefits of transdermal patches, patients often appreciate predictable dosing, reduced GI effects, and improved convenience. Looking at common uses of transdermal patches, clinicians reference roles in pain control, smoking cessation, and hormone replacement, among others. Emerging research in microneedle arrays and smart adhesives signals a future where these systems become more personalized and safer for diverse groups.
How Transdermal Patches Work: Mechanisms and Drug Delivery
How transdermal patches work is grounded in a simple principle: the drug is embedded in a matrix or reservoir within the patch and diffuses slowly through the skin’s outer layer, the stratum corneum, into the bloodstream over hours or days. This design enables controlled release and steady exposure, which helps avoid the peaks and troughs seen with some oral therapies.
By bypassing the digestive system and first-pass metabolism by the liver for many medications, transdermal delivery can improve bioavailability and reduce stomach-related side effects. The patch’s outer layer acts as a rate-controlling barrier, and the drug then travels through the skin to reach systemic circulation, yielding predictable therapeutic levels.
Types of Transdermal Patches: Matrix vs Reservoir and Drug Examples
Types of transdermal patches include matrix-type and reservoir-type designs, each with distinct release mechanisms and clinical implications. Matrix patches embed the drug within a solid or gel matrix, creating a controlled diffusion gradient that releases medication steadily.
Common examples span nicotine patches for smoking cessation, fentanyl patches for chronic pain, scopolamine patches for motion sickness, and hormone patches for replacement therapy. The choice between matrix and reservoir formats affects release rate, skin tolerance, wear time, and patient comfort.
Benefits of Transdermal Patches for Patients
Benefits of transdermal patches include non-oral dosing, steady plasma levels, and improved adherence for once-daily or longer-interval therapies. This delivery method can be especially advantageous for people with swallowing difficulties, nausea, or poor tolerance for oral medications.
Because many drugs experience first-pass metabolism, transdermal delivery can improve systemic bioavailability and minimize GI irritation, making it suitable for patients who need reliable, sustained exposure without relying on the digestive system.
Common Uses of Transdermal Patches Across Therapies
Common uses of transdermal patches span smoking cessation, chronic pain management, motion sickness prevention, and hormone replacement therapy. Nicotine patches provide a steady nicotine level, while fentanyl patches offer continuous analgesia, and scopolamine patches help prevent motion sickness.
Hormone patches deliver estrogen or testosterone for replacement therapy, aiding menopause symptoms or hypogonadism, while local anesthetic patches like lidocaine provide targeted relief near the application site without systemic effects. The range of drugs suitable for transdermal delivery continues to expand as patch design advances.
Care and Safety of Transdermal Patches: Skin Health and Safe Use
Care and safety of transdermal patches focus on protecting the skin and maintaining safe drug exposure. Choose a clean, dry site, rotate locations to minimize irritation, and monitor for redness, itching, or persistent irritation.
Heat and sweating can increase absorption, so avoid hot baths or saunas during wear. Do not cut patches without clinician approval, and wash hands after applying or removing to prevent transferring medication to others. Some patches require removal before MRI or certain medical procedures; follow label directions or clinician guidance in these cases.
Practical Guidelines: Applying, Maintaining, and Monitoring Your Patch
Proper application improves delivery and comfort. Start with clean, dry, intact skin; avoid irritated or recently shaved areas. Remove the patch’s backing, center it on the chosen site, and press firmly at the edges for 20–30 seconds to ensure adherence.
After removal, fold the patch with the sticky sides together for disposal and wash your hands. If the patch begins to peel or curl, change to a new site at the next scheduled replacement, and monitor for any skin reactions or changes in how the patch adheres throughout the wear period.
Frequently Asked Questions
How do transdermal patches work and why is this mechanism important?
Transdermal patches deliver medicine through the skin into the bloodstream over hours to days by embedding the drug in a matrix or reservoir. They bypass the digestive system and first-pass metabolism, promoting better bioavailability and steadier drug levels. This steady release reduces peaks and troughs, supports convenient dosing, and can improve tolerability for certain medications.
What are the types of transdermal patches and how do they differ?
Transdermal patches include matrix-type patches, which embed the drug in a solid or gel matrix for controlled diffusion, and reservoir-type patches, which hold a liquid drug reservoir for flexible release. Common examples include nicotine patches, fentanyl patches, scopolamine patches, hormone patches, and local anesthetic patches like lidocaine. Differences in release rate, adhesion, wear time, and skin tolerance influence choice.
What are the benefits of transdermal patches?
Benefits include non-oral dosing, steady plasma levels, reduced stomach-related side effects, and avoidance of first-pass metabolism for eligible drugs. Patches can improve adherence with once-daily or longer-interval dosing and are suitable for people who have difficulty swallowing or experience GI intolerance.
What are common uses of transdermal patches?
Common uses include nicotine patches for smoking cessation, fentanyl patches for chronic pain, scopolamine patches for motion sickness, hormone patches for estrogen or testosterone replacement, and lidocaine patches for local relief. Ongoing research is expanding patches to cover additional conditions.
What care and safety steps are essential when using transdermal patches?
Apply patches to clean, dry skin on an appropriate site, rotate locations to minimize irritation, and avoid hair, lotion, or broken skin. Heat and sweating can increase absorption, so avoid hot baths or saunas during wear. Do not cut patches unless advised, wash hands after handling, and follow disposal guidelines. Some patches require removal before MRI or certain procedures.
How should I assess suitability and talk with a clinician about transdermal patches?
Discuss your medical history, current medications, allergies, and skin health with your clinician to determine if transdermal delivery is appropriate. They will review expected duration, benefits, and risks, and help monitor for skin reactions, drug interactions, and adherence. Active participation helps tailor therapy and safety for your needs.
| Topic | Key Points |
|---|---|
| What are transdermal patches? | Thin, adhesive devices delivering drugs through the skin into the bloodstream; provide steady release over roughly 24–72 hours; bypass the digestive system and first-pass metabolism for many drugs, improving bioavailability. |
| How they work | Drug is embedded in a matrix or reservoir; applied to clean, dry skin; diffusion through the stratum corneum to reach systemic circulation; results in smooth, sustained drug presence rather than rapid spikes. |
| Types | Matrix-type patches embed drug in a solid/gel matrix; reservoir-type patches contain a liquid drug reservoir; examples include nicotine, fentanyl, scopolamine, and hormone patches; design affects release rate, skin tolerance, and wear time. |
| Benefits | Non-oral dosing; steady plasma levels; improved adherence with once-daily or every-48-hours dosing; avoids GI irritation; potential for better bioavailability for drugs with extensive first-pass metabolism. |
| Safety and care | Choose clean, dry skin; rotate sites; monitor for redness or irritation; heat can increase absorption; do not cut patches unless advised; wash hands after handling; some patches require removal for MRI or procedures. |
| Applying and maintenance | Apply to clean, dry skin; avoid irritated or recently shaved areas; remove backing, center patch, press edges for 20–30 seconds; folded sticky sides together for disposal; if peeling occurs, switch sites at next replacement. |
| Common uses | Nicotine patches for smoking cessation; fentanyl patches for chronic pain; scopolamine for motion sickness; hormone patches (estrogen/testosterone); lidocaine patches for local analgesia; broader uses continue to expand with patch design. |
| Limitations and considerations | Not all drugs pass easily through the skin; some patches may irritate skin; adhesion affected by sweating, swimming, or fabrics; potential drug interactions; consult clinician to assess suitability. |
| Future directions | Microneedle patches for more precise dosing with less discomfort; smart patches with sensors to monitor drug levels or vital signs; improved adhesives and flexible substrates for better wear and acceptance. |
| Clinician discussion and assessment | Discuss medical history, medications, and lifestyle with a clinician to determine suitability, duration, and risks; report skin reactions promptly and use patches as directed to support safety and efficacy. |
Summary
Transdermal patches (transdermal patches) are a versatile, patient-friendly drug delivery system that can provide steady medication levels with convenient dosing. They deliver medicine through the skin into the bloodstream, bypassing the digestive system and first-pass metabolism in many cases, which can improve bioavailability and minimize GI side effects. With both matrix-type and reservoir-type designs, transdermal patches offer varied release rates and wear times to suit different therapies. Proper skin care, correct application, and ongoing monitoring help maximize safety and efficacy. As research advances, innovations like microneedle patches and smart sensor-enabled patches may expand the range of conditions that can be treated with transdermal patches, bringing smarter and more personalized delivery options to patients.